Compressed Air Best Practices interviewed Robert G. Beierle, P.E., Senior Associate, of BSA LifeStructures.
Good afternoon. Please describe BSA LifeStructures and what businesses it is in.
Good afternoon. BSA LifeStructures is a full service architectural and engineering firm specializing in healthcare, higher education and technology facilities. We employ close to 260 associates and are established in two locations; Indianapolis and Chicago. We were founded over thirty years ago. Our strongest focus is on hospitals and university facilities.
 What kind of hospitals do you work with?
What kind of hospitals do you work with?
We work with every kind of healthcare facility you can imagine. We design brand new hospitals from scratch and we also design additions to existing hospitals. We have recently, for example, done a lot of additions to hospitals that have acquired the capability to do MRI and CAT Scan work. We also do many renovations in hospitals that need to upgrade their installations and bring them up to code. This often includes medical gas systems.
How does BSA LifeStructures get involved with compressed air systems in hospitals-what is your role in the process?
We design medical air systems for hospitals. We have worked for years with compressed air systems and are very familiar with the NFPA guidelines. Our role in the process depends upon the project. When doing an addition to a hospital, we will evaluate the existing compressed air system to see if more capacity is needed. Some hospitals call us to come in and see if their medical gas system is up to code (the current NFPA code). The compressed air system is an important part of this survey. We will visit the hospital and do a survey. Some of these projects result in a complete system replacement and some result in the addition of some specific components, like CO Monitors or Dew Point Monitors.

How do you decide how much air is needed?
BSA LifeStructures does engineering work for hospitals to create a medical gas system that suits their needs. Our engineering and architectural teams will meet with each of the different types of occupancies in the hospital to determine their needs with medical gases. How many beds do they have? How many respirators? How many incubators? A key question is, what is the “simultaneous use factor” that they want to use in that area of the hospital? We recently, for example, worked with a 75-bed neonatal intensive care unit. They asked us to size their occupancy area for 100% simultaneous usage. This meant that they wanted to be able to support all 75 beds, at the same time, if necessary. We will then calculate the compressed air demand, in scfm, per bed and multiply it times the usage factor.
We offer the nurses and doctors advice on the usage rates we typically see in their areas, but it is ultimately their decision. We will also speak with the engineering and facility management, at the hospital, to hear their experience with the different occupancy area. At the end of these meetings and discussions regarding medical gas usage, we will be able to create a demand curve for compressed air. We can then proceed with preparing drawing and specifications for equipment and pipelines.
In a hospital, because there are so many types of areas, the simultaneous use factor gives us a demand curve. As an example, the 75-bed NICU could have a capacity of 75 infants, so we sized for 100% simultaneous use factor. We spend a lot of time, in the design phase, speaking with nursing staff, doctors involved in the unit, and with engineering/facility services to get input on the use factor of this area of the hospital. This is what our engineering and architectural teams do in many meetings.
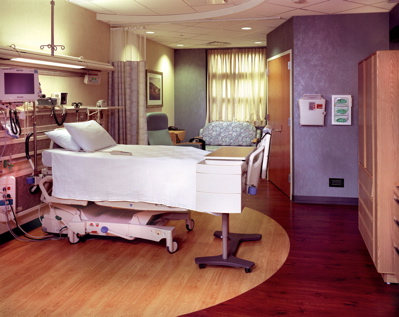
Medical compressed air systems are often used in intensive care units. Dan Francis, Mardan Photography
Which areas, in a hospital, see a lot of compressed air use?
The biggest area is in the neonatal intensive care units. Infants are in incubators and are completely reliant upon the supply of breathing air. The pediatrics areas, particularly in winter, also require the use of many respirators to assist children with the flu or with asthma. A number of hospitals are also putting in contamination wash-down areas to cleanse people who have become exposed to a hazardous contaminant. They need an area where they can hose these patients down while protecting themselves with a hood, body-suit, and a respirator.
What kinds of air compressors does BSA LifeStructures recommend to hospitals?
We started, years ago, with the Nash oil-free air compressors and have been using, over the past few years, oil-less reciprocating air compressors.
We’ve just been introduced to the new oil-free rotary-tooth air compressors and think it will be our next step. The NFPA 99 Code approved rotary compressors as an oil-free technology, recently, and we like the reduced maintenance this technology offers. The only moving parts are the lubricated bearings and they can run a lot longer with only doing the recommended oil change on the gear box. This is less maintenance than with the oil-less reciprocating compressors, where the manufacturers recommend a “tear-down” every 20,000 hours to check the pistons, rings, and bearings. We have a lot of hospitals whose maintenance departments have been reduced. Some surgery centers don’t have their own maintenance and have to outsource it. All of our customers are looking for ways to reduce maintenance requirements.
We also recommend scroll compressors for smaller applications. They are compact and are easy to offer in duplex and multiplex configurations.
The sizes of the packages vary from job-to-job. We run from very small projects to very large. The neonatal intensive care unit I referred to earlier required six (6), twenty (20) horsepower air compressors.
What kinds of air dryers does BSA LifeStructures recommend to hospitals? Why?
Technology has also evolved with compressed air dryers. We will size a compressed air dryer, which can handle the combined installed capacity of the air compressors. This assures the hospital of air treatment under peak usage conditions. We used to recommend refrigerated air dryers, but we now recommend desiccant air dryers. All of the compressor packagers have moved in the direction of duplex desiccant air dryers for the primary and standby drying systems. NFPA 99 changed the dewpoint requirement to 32 F and the industry has moved in this direction. If a hospital has serious budgeting issues, we sometimes recommend a refrigerated dryer as the standby drying system behind a desiccant air dryer.
What operating pressures are common in hospitals?
Operating pressure is normally at 55 psig delivered to the hospital. We allow for a five-pound (5 psig) pressure drop through the piping and deliver air at 50 psig to the outlets. The air compressors are normally delivering compressed air at 100 psig to the compressed air dryers. After the dryers, a set of duplex regulators bring the air pressure down to 55 psig.
Why is the air compressed at 100 psig for a 50 psig application?
That is a good question. The answer lies with the capabilities of the oil-free air compressor technologies that we have available to meet the NFPA Code. I’m sure energy savings could be achieved if we compressed the air at a lower pressure.
What can the compressed air industry do to help hospitals?
The industry is doing a good job of coming out with new technologies-like this new rotary tooth compressor. We are seeing advancements in designs, which offer benefits to the hospitals that are real – like reduced maintenance. The scroll compressors were introduced to hospitals, only a few years ago, and they have also provided reduced maintenance benefits. The air drying systems have also evolved from refrigerated to desiccant air dryers. CO and dewpoint monitoring is seeing better compliance every year. The industry has done a good job of increasing awareness of this issue. Hospitals now go to the equipment vendors and have gone ahead and upgraded their systems on their own by having these monitors installed.
What are the main issues facing hospitals with compressed air systems?
Older facilities are wearing out their equipment and need to replace it. They are always fighting fund allocation issues to get it done. It gets put off and put off until it has to be done. These situations can be hard to deal with. You have to replace all the air compressors – but you can’t turn off the supply of compressed air, to the hospital, while you do it! Sometimes the hospital can create more room, in the compressor room, by removing other equipment. We can then bring in the new equipment while the old equipment is still running. Sometimes we have to bring in a rental air compressor, to supply the hospital while we do the project to remove the old and bring in the new equipment.
Another major issue we face is how to source clean ambient air for the air compressor intakes. The air compressors are usually located in the basement and we have to run pipe 2-3 stories up to the roof to access clean ambient air. On the roof we compete with the boiler stacks, which are discharging flu gases, with air handling intakes, and with helipads! We also have to take into consideration wind currents and what the wind brings with it. We are currently working on a system that is four blocks away from the smokestacks of an industrial facility. We have engaged a firm, whose expertise is with wind currents, to take all of these factors into consideration and to advise us on where to locate all of these things on the roof of the hospital. As you can see, it isn’t so easy to access clean ambient air.
Thank you BSA LifeStructures for your insights.
For more information, please contact Mr. Robert Beierle, BSA LifeStructures, email: rbeierle@bsalifestructures.com, tel: 317-819-7878, www.bsalifestructures.com.
For more articles about Medical Air Standards, visit www.airbestpractices.com/standards/nfpa-99-medical-air.